Many men over 40 overlook the core reason behind a weak urine stream: Benign Prostatic Hyperplasia (BPH). This isn't just a natural part of aging; it's a common condition causing structural issues that significantly impact quality of life. In Korea, like elsewhere, BPH, prostatitis, and even prostate cancer can co-occur in men over 40, making accurate diagnosis and management crucial. This guide provides the latest 2026 information on BPH symptoms, progression, diagnostic criteria, treatment options, and insurance coverage relevant to US patients.
What Causes BPH? Understanding the Structural Issues
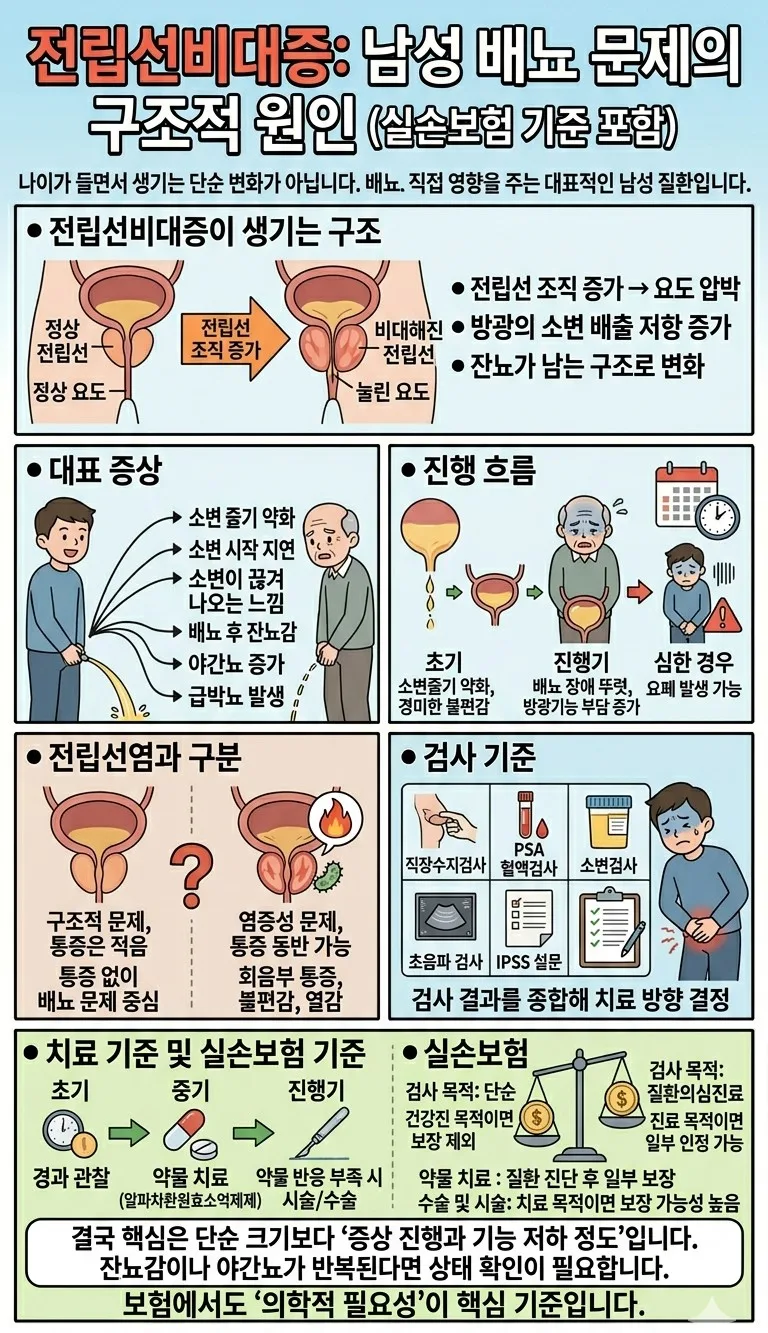
The prostate gland sits just below the bladder, encircling the urethra (the tube that carries urine out of the body). As men age, particularly after 40, the prostate tissue can enlarge, a condition known as BPH. This enlargement squeezes the urethra, narrowing the passage for urine. Consequently, the bladder has to work harder to push urine through, leading to incomplete emptying and residual urine. This is a structural problem, distinct from cancerous growths, but it significantly hinders urinary flow. Many middle-aged men notice a weaker stream because of this urethral compression. The prostate's increased size directly obstructs the urethra, making it harder for urine to pass freely, a primary driver of urinary symptoms.
Key Symptoms of Benign Prostatic Hyperplasia (BPH)
BPH typically manifests as a cluster of urinary symptoms rather than a single issue. The most common complaints include a weak or slow urine stream and difficulty initiating urination. You might also experience urine flow that stops and starts, a persistent feeling of incomplete bladder emptying (residual urine), frequent nighttime urination (nocturia), and a sudden, urgent need to urinate that's hard to control (urinary urgency). While these symptoms can sometimes be mistaken for bladder problems, they are often rooted in the urethral compression caused by an enlarged prostate. Recognizing these signs early is vital for effective management and preventing further complications.
How BPH Progresses: Stages and Management Strategies
Benign Prostatic Hyperplasia generally progresses slowly, with symptoms evolving over time. In the early stages, you might only notice a slightly weaker urine stream or minor discomfort. However, as the condition advances to the moderate stage, the feeling of residual urine becomes more pronounced, and nocturia increases, disrupting sleep patterns. In the advanced stages, urinary dysfunction can become severe, placing significant strain on the bladder and potentially leading to serious complications like acute urinary retention, where you can't urinate at all. Given the substantial impact on daily life, especially from disrupted sleep due to nocturia, proactive management is essential from the moderate stage onwards.
Differentiating BPH from Prostatitis: Understanding the Differences
It's common to confuse BPH with prostatitis, as both affect the prostate gland. However, they stem from different causes and present with distinct symptoms. BPH is primarily a structural issue caused by prostate enlargement leading to urethral obstruction, typically with less associated pain. Prostatitis, on the other hand, is an inflammation of the prostate, often due to infection, and is frequently accompanied by pain in the perineum, discomfort, and sometimes fever. If you're experiencing primarily urinary flow issues without significant pain, BPH is more likely. However, if pain or inflammatory symptoms are present, prostatitis should be considered. Accurate diagnosis by a healthcare professional is key to determining the correct course of treatment.
When is Medical Intervention Necessary for BPH?
The decision to treat BPH isn't solely based on prostate size; it's primarily driven by the severity of your symptoms and the presence of complications. Mild symptoms that don't significantly impact your daily life might be managed with watchful waiting and lifestyle adjustments. However, if symptoms like a weak stream, nocturia, or urgency interfere with your quality of life, or if complications such as urinary tract infections, bladder stones, or kidney damage arise, medical intervention becomes necessary. Your doctor will assess your specific situation, considering symptom scores and potential complications, to recommend the most appropriate treatment path, which could include medication or surgical options.
Navigating Health Insurance for BPH Treatment in the US
For US patients, understanding health insurance coverage for BPH is crucial. Most health insurance plans, including PPO, HMO, and Medicare, cover medically necessary treatments for BPH. This typically includes diagnostic tests like PSA blood tests and ultrasounds, prescription medications (like alpha-blockers or 5-alpha-reductase inhibitors), and surgical procedures such as TURP (Transurethral Resection of the Prostate) or minimally invasive options. The key is that the treatment must be deemed medically necessary by your physician. Routine check-ups or preventative screenings not directly related to diagnosed symptoms might have different coverage rules. Always verify your specific plan benefits and deductible requirements with your insurance provider before undergoing treatment.
Tags
Original Source
Read the Korean original