Your actual reimbursement for outpatient medical visits under a Korean national health insurance plan can vary significantly, even for the same treatment. Key factors influencing the final amount you receive include whether claims were missed, the completeness of your submitted documentation, the specific terms of your policy based on when you enrolled, and how the insurance company processes your claim. The inclusion of non-covered (비급여) services also plays a crucial role in determining your out-of-pocket expenses and the final reimbursement amount.
Why Does Outpatient Reimbursement Vary So Much?
The perceived difference in reimbursement amounts for outpatient medical visits, even when the services rendered are identical, often stems from various structural factors within the claims process rather than a change in the core payment standards. When you actually file a claim, you might notice that missed receipts for prescriptions or tests, incomplete documentation, or a high proportion of non-covered services directly impact the amount you get back. Furthermore, the policy terms you agreed to when you first enrolled significantly influence your coverage scope and deductible amounts, leading to different reimbursement experiences for individuals who joined at different times.
What Factors Influence Outpatient Medical Reimbursement?
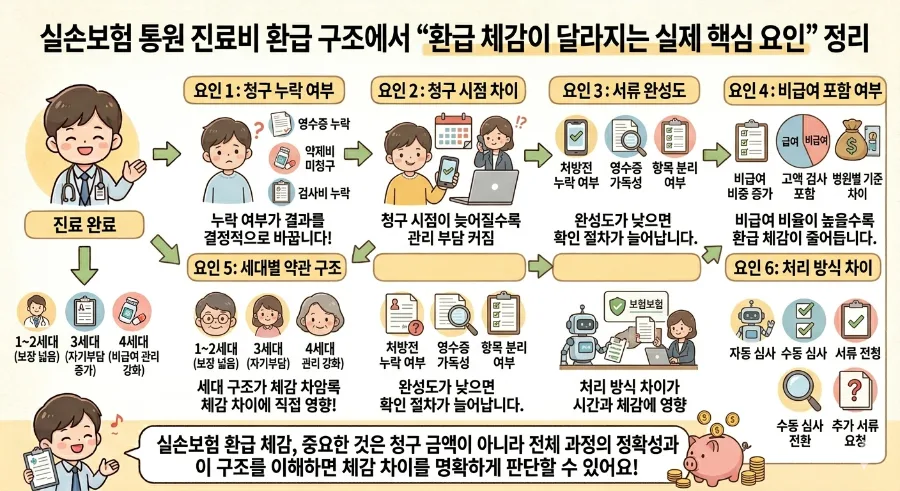
When filing a claim for outpatient medical expenses, several factors can influence the reimbursement amount you ultimately receive. These can be broadly categorized into six key areas. Firstly, any missed claims for receipts, prescription costs, or test fees mean you won't be reimbursed for those specific amounts, directly reducing your overall payout. Secondly, the timing of your claim submission can matter; immediate claims might be easier to manage than delayed ones. Thirdly, the completeness and clarity of your submitted documents are crucial. Missing doctor's notes, illegible receipts, or poorly itemized expenses can delay the insurance company's review process or lead to requests for additional information. Fourthly, the inclusion of non-covered (비급여) services often increases your out-of-pocket responsibility, as these typically have higher co-payment rates, thus reducing the perceived reimbursement. Fifthly, the generational policy structure you are under plays a significant role; early policies (1st-2nd generation) generally offered broader coverage, while later policies (3rd and 4th generation) introduced higher deductibles and stricter management of non-covered services. Finally, differences in how insurance companies process claims—whether through automated systems, manual reviews, or requiring supplementary documents—can affect the speed and outcome of your reimbursement.
What Should You Watch Out For When Getting Reimbursed?
When seeking reimbursement for outpatient visits, the most critical aspect is ensuring the completeness and accuracy of your claim submission. It's not just about the total amount spent; it's about ensuring all relevant medical records, receipts, and prescription slips are submitted without any omissions. For non-covered services, which often come with higher co-payment percentages, it's wise to understand which services fall into this category and to review your insurance policy's specifics beforehand. This is especially important for high-cost tests or treatments. Additionally, understanding your specific policy's generation is key to knowing your coverage limits and deductible percentages. For instance, under the 4th generation policy, excessive use of non-covered services might even lead to premium increases, making it prudent to avoid unnecessary treatments. Since reimbursement amounts can vary based on individual policy terms and treatment details, consulting with your insurance provider or a financial expert is recommended for precise guidance.
What Are Common Mistakes in Outpatient Reimbursement Claims?
A frequent mistake many individuals make during the outpatient reimbursement process is failing to submit all necessary documentation. This often includes overlooking prescription receipts, doctor's notes, or lab test results, which can lead to receiving less than the eligible amount. Furthermore, submitting documents that are difficult to read or lack clear itemization can prolong the insurance company's review and potentially lead to requests for additional paperwork, causing inconvenience. Another common pitfall is underestimating the impact of non-covered services; individuals may be surprised by lower-than-expected reimbursements because these services carry higher personal cost-sharing. Lastly, a lack of familiarity with one's own insurance policy is a significant oversight. Since deductibles and coverage scopes differ across policy generations (e.g., 1st-4th generation), understanding these specifics is crucial for accurate claim submissions and managing expectations. To avoid these errors, always double-check all submitted documents and familiarize yourself with your policy's terms before filing.
For more details, check the original source below.





